Case 1: This is a 10 month old boy who has had crossed eyes since birth.
He cross-fixates, and does not object to occluding either eye. His ocular exam is otherwise normal, and his cycloplegic refraction is +1D in both eyes. His alignment is stable from his initial exam 2 months ago. You estimate he is ET 40 by Krimsky. What is your surgical plan?
Case 2: This is a 12 year old girl who has been concerned about her friends noticing her eye drifting.
You find her acuity to be 20/20 in both eyes without correction. Her X(T) measures 45PD, she becomes tropic spontaneously, and will often remain tropic through a blink. Her stereoacuity has decreased over the past 6 months from 40 sec to 200 sec. What is your surgical plan?
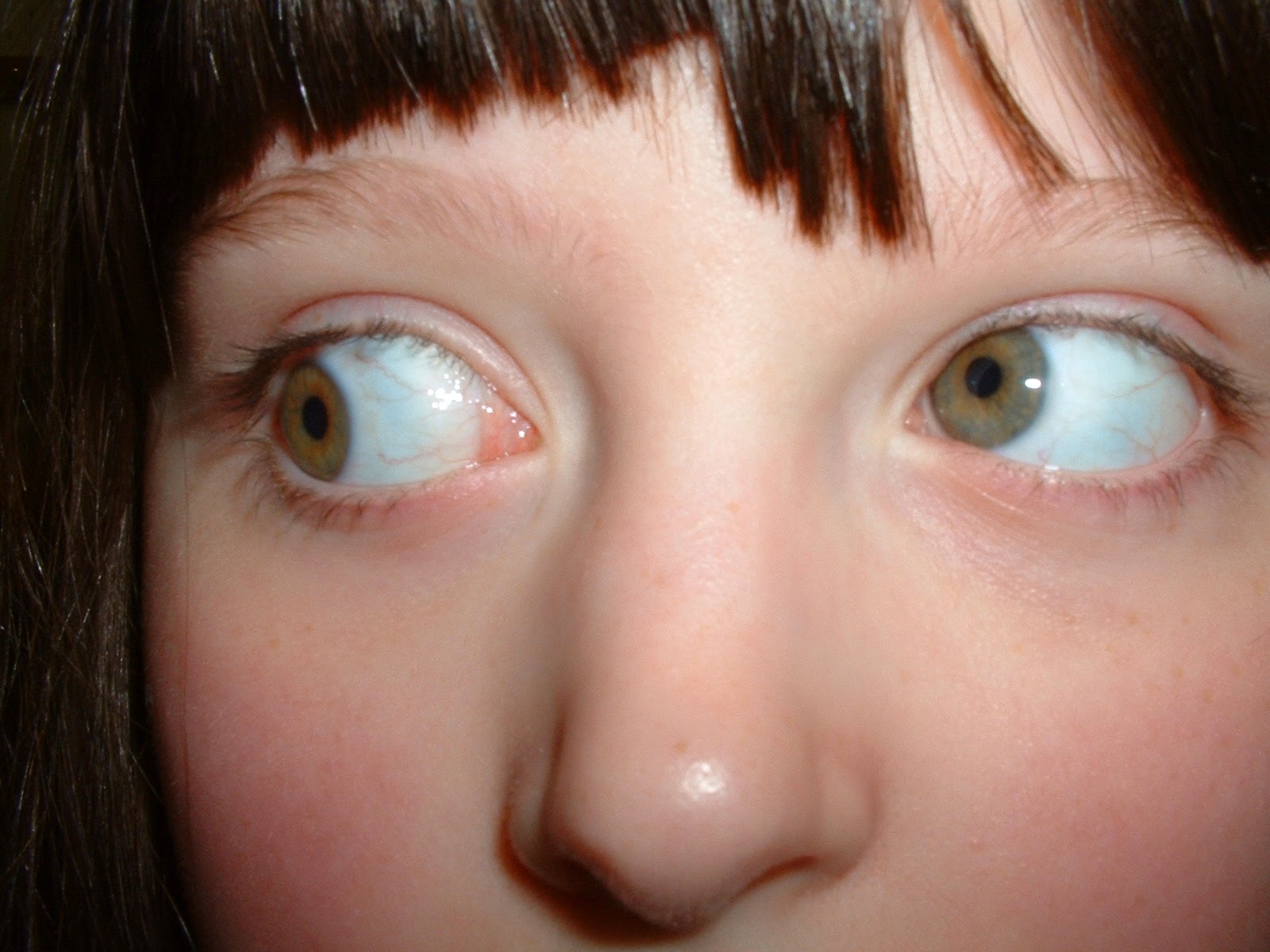
Case 3: This is a 7 year old girl, who had surgery for esotropia when she was 8 months old. For the past year, she has been turning her face to the right, and sometimes adopting a small tilt to the right.
Her acuity is 20/20 in both eyes without correction. You measure LHT 6 in forced primary gaze, LHT 15 in right gaze, Ortho in left gaze and downgaze. Her LHT increases on left head tilt. What is your surgical plan?




Tai's and Rachel's plans:
ReplyDelete1. congential esotropia, maximal medial rescession consider subsequent lateral resections if residual ET
2. exotropia: Bilateral lateral rectus recession
3. Inferior oblique overration - inferior oblique myotomy
Liegel
ReplyDeleteCase 1: bilateral medial rectus recession
Case 2: bilateral lateral rectus recession
Case 3: left inferior oblique myotomy vs left superior oblique tuck
Case 3: SO tuck appropriate if torsion is a big concern, or if marked limitation to depression in adduction. It may cause iatrogenic Brown's; it's possible to adjust, but not as easy as contralateral IR.
DeleteCase #1: RMR recession, RLR resection
ReplyDeleteCase #2: LLR recession
Case #3: Left Inferior oblique myectomy (for L superior oblique palsy), possible L SR recession.
Case 2: May be able to get by with just 1 lateral, but large unilateral recession may lead to more incommitance after surgery than bilateral symmetric surgery.
DeleteCase 3: Ipsilateral SR recession may lessen the improvement in incommitance that the IO weakening provides (i.e. may end up with LHT in right gaze, ortho in primary, and RHT in left gaze). SR recession may be a good option if the LHT was commitant to start, or if there was restriction to depression on forced duction from SR contracture.
1) Bilateral medial rectus recession 9 mm
ReplyDelete2) Left LR recession 8 mm and MR resection 6 mm.
3) Left Inferior Oblique Myectomy
Thanks.
~Anushree
Good plans (the maximal recession of MR is usually 6-7mm, so 9mm is likely to lead to limitation of adduction post-op)
Delete